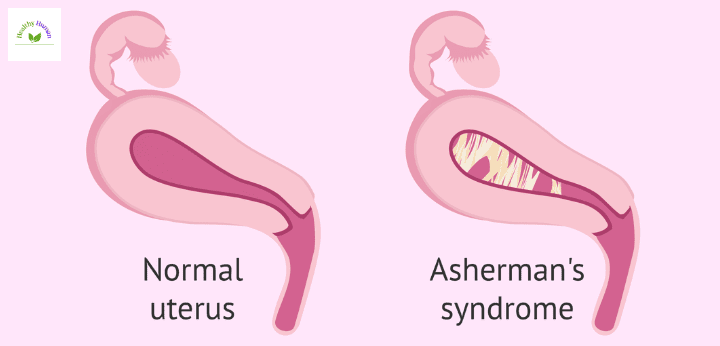
Asherman’s syndrome is a female-specific disorder that can occur. It is classified as a rare gynecological condition that affects the female reproductive system. Scar tissue forms in the uterus or cervix as a result of the disorder. Because of the scar tissue, the uterine walls thicken. They take up more room than usual, making the uterus smaller in size.
The walls can fuse together in severe circumstances. Intrauterine adhesions is another name for the condition. Because Asherman’s syndrome has not usually identified, it is difficult to estimate how common it is.
How Does Asherman’s Syndrome Affect Fertility?
If you have Asherman syndrome, you may find it difficult to conceive. If you do, your chances of miscarriage are high. It is possible to become pregnant while suffering from the illness, but the adhesions in the uterine walls do not allow for foetal development. This increases your odds of having a miscarriage or stillbirth compared to women who do not have the disorder.
Asherman syndrome has also associated with an increased risk of several pregnancy-related disorders, including:
- Placenta Increta- The placenta juts excessively far into the uterine wall. As a result, a high-risk pregnancy occurs. After delivery, all or part of it stays connected, causing excessive bleeding.
- Placenta Previa- The placenta closes the cervix, causing heavy bleeding throughout pregnancy and delivery. It also raises the possibility of preterm delivery.
- Excessive Bleeding- It can cause miscarriage, infection, or be a symptom of an ectopic pregnancy. An ectopic pregnancy is one that occurs in your fallopian tube.
Although Asherman syndrome is not a life-threatening disorder, it can lead to recurrent miscarriages. If you have Asherman syndrome, make sure you see your doctor on a regular basis so that they can monitor your pregnancy.
Causes of Asherman’s Syndrome
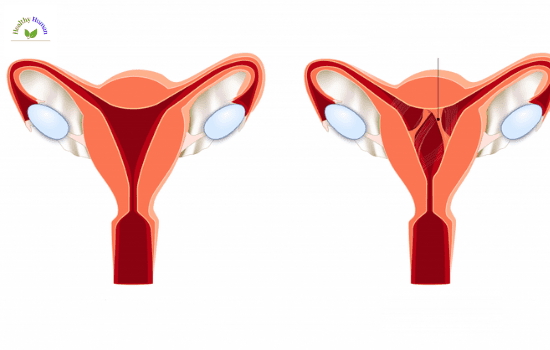
The most common cause is surgical scraping or washing of tissue during a dilatation and curettage procedure (D&C). The operation may often performed following an elective abortion, a miscarriage, or the removal of a retained placenta after delivery. The damage to the uterine walls as a result of the surgery produces a scar.
If you have surgery to remove a retained placenta between two and four weeks after giving birth, you have a 25% chance of getting Asherman syndrome. When the placenta does not exit your body within 30 minutes after giving delivery, it has said to retained. It can occur if it becomes caught behind the cervix or becomes attached to the uterine wall. The more of these treatments you undergo, the more likely you are to have the disorder. Uterine adhesions can also caused by other pelvic procedures, such as a cesarean section or fibroids excision.
Endometrium infections, such as genital TB, are another reason. When TB germs invade your reproductive system, you have genital tuberculosis.
Asherman syndrome situations differ from person to person, thus determining your cause should do on a case-by-case basis. There is a form of condition in which the uterine walls do not adhere together. Instead, the endometrium has exposed due to the removal or destruction of the basal layer. Radiation therapy may potentially induce Asherman syndrome.
Also Read:- Sexual Dysfunction & Disorders In Men
Symptoms of Asherman Syndrome
The most prevalent sign of Asherman syndrome is a lack of or inability to get periods. You may also have discomfort when your period is due but there is no blood. This might indicate that you’re on your period, but blood is unable to escape your uterus due to the obstruction.
- Other causes, however, might lead you to miss your period, such as:
- Menopause
- Over-exercising
- Stress
- Rapid weight reduction
- Using birth control or the contraceptive pill
- Polycystic ovarian syndrome (PCOS)
Consult your doctor if your menstruation becomes irregular or uncommon. The cause might be something else that needs treatment.
In other circumstances, your periods may be regular or extremely erratic. Other signs of Asherman syndrome include infertility and repeated miscarriages.
Prognosis of Asherman Syndrome
Although Asherman’s syndrome is not fatal, some women who have it are unable to conceive or have repeated miscarriages. Women with Asherman’s syndrome have a greater chance of miscarriage and stillbirth. Women with this illness are also more likely to experience prenatal hemorrhage. Fertility can recovered if the condition may addressed.
Diagnosis of Asherman Syndrome

Your doctor will collect a detailed medical history and do a physical examination. A physical exam will only use in exceptional circumstances to detect adhesions. If a medical device can inserted and is unable to enter the cervix, they may discover cervical obstruction.
They will also do a blood test to rule out any other underlying diseases that may be causing these symptoms. An ultrasound will also reveal the thickness of the uterine wall and the number of follicles.
Ultrasonography
Ultrasonography, sometimes known as ultrasonography, is a diagnostic technique that produces images of the inside of the body. To view this cavity, transvaginal ultrasonography must place into the vagina and into the uterus.
This id often done in the first instance because it is easy, non-invasive, and may be done during a consultation. However, because of the difficulties in interpreting the pictures acquired, their conclusions are not always definitive. As a result, more specialist approaches are must required.
Hysteroscopy
Another option is to dilate your cervix and implant a tiny telescope-like hysteroscope. The doctor will examine the interior of your uterus for scarring. The procedure is call a hysteroscopy.
Finally, if the diagnosis remains ambiguous after the above investigations, a diagnostic hysteroscopy may done. This procedure involves placing a camera into the uterine cavity and observing it.
The identification of Asherman’s syndrome is significantly clearer with this test since the adhesions have more directly visualised. This is why hysteroscopy is the best approach for diagnosing it.
Hysterosalpingogram (HSG)
They may combine this with a hysterosalpingogram (HSG), in which a particular dye can inserted into the uterus. An X-ray helps reveal all abnormalities within the uterine cavity, including obstructions and growths.
A radiograph is paired with the use of a contrast liquid in this medical diagnostic. This fluid is critical in this test because it enters the uterus and extends throughout the cavity until it reaches the fallopian tubes and is discharged into the peritoneal area. The contrast agent “draws” the outline of the uterus and tubes in this way. An x-ray is obtained after the contrast has been injected.
The presence of adhesions, blockages, or changes such as fibroids or polyps is simpler to identify with a hysterosalpingogram than with an ultrasound.
Although it does not require anesthetic and is not very painful, it is a complex surgery that must be arranged and carried out in a specialist facility.
Treatment
Surgery is frequently used to treat Asherman syndrome. The scar tissue or adhesions will be taken away by the surgeon. The operation is non-invasive and performed via hysteroscopy. You will be sedated, and oestrogen may be provided following surgery to improve the health of your uterine lining. Allow 12 months for the scar to heal before attempting to conceive.
Prevention
The D and C technique is the best strategy to avoid Asherman syndrome. Following a missed or partial miscarriage, retained placenta, or postpartum hemorrhage, most women should be able to select medical evacuation.
If a D & C is necessary, the surgeon can use an ultrasound to guide them and limit the chance of uterine injury.
Conclusion
Asherman syndrome can make conception difficult, if not impossible, to conceive. It may also raise your chances of having major issues throughout your pregnancy. The disease is frequently treated as well as prevented.
If you have Asherman syndrome and your fertility cannot be restored, contact a support organization such as the National Fertility Support Center. Women who want children but are unable to conceive have choices. Surrogacy and adoption are two of these alternatives.
Also Read:- Gaming Addiction-All You Must Know About Negative Impact
Also Read:- Effective Ways to Improve the Male Fertility




