Breasts are made up of fatty tissue. Breast milk is produced in small chambers known as lobules. To reach the nipples, milk travels through tiny channels known as ducts. Lymph nodes are inside your breasts and beneath your arms. They are connected with lymph vessels and help to fight body disease. Now, let’s just learn about what is breast cancer, how it affects the body parts, and how can we prevent it from spreading.
What is Breast Cancer?
Breast cancer develops when healthy breast cells become abnormal, multiply uncontrollably, and form tumors. It can spread to other regions of the body at times. About 1 in 8 women have a lifetime risk of having breast cancer. For men, the risk is 1 in 1000. Breast cancer that develops inside the ducts is called Ductal carcinoma in situ or DCIS. When DCIS spreads into the surrounding tissue, it is called Invasive carcinoma or IDC. Abnormal cells can form in the breast lobules. They are known as lobular carcinoma in situ or LCIS. When these cells spread in the surrounding tissue, they become cancer called Invasive lobular carcinoma.
Signs of breast cancer
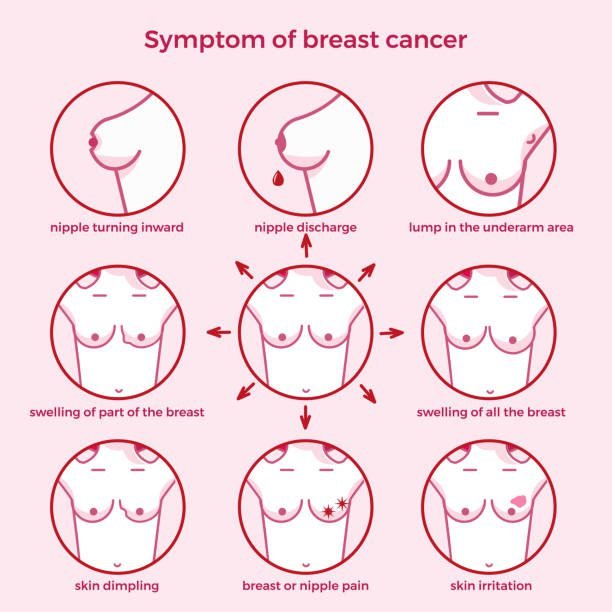
- Lump
Breast lumps are common, and the majority of them are harmless (noncancerous), especially in younger women. Even so many breast lump a doctor can investigate, — particularly if it’s new, feels different from your other breast, or is different from what you’ve felt in the past.
- Nipple discharge
The discharge may consist of anything other than breast milk and usually occurs without the squeezing of the breast or only on one breast.
- Skin changes red or inflamed
Redness, or thickening of the nipple or breast skin
- Skin changes skin dimpling
This discomfort and dimpling are sometimes referring as having the appearance of an orange peel.
- Lymph nodes under the arm or around the collarbone that are swollen.
Breast tissue extends under the arms and into the collarbone, and breast cancer can sometimes spread to the lymph nodes in these areas before the original breast tumor is large enough to be felt.
- Swelling of the entire or a portion of the breast
Even if you don’t feel a distinct mass or lump, if you notice swelling in any part of your breast, it could be breast cancer.
Risks factors for breast cancer

- Older age
If you’re 55 or older, you’re more likely to develop breast cancer.
- Dense breasts
Cancers can be difficult to detect on mammography because dense breasts have more connective tissue than fatty tissue. Women with thick breasts are more likely to develop breast cancer.
- Having breast cancer before
Women who had this before are more likely to have it again. Non-cancerous breast illnesses such as atypical hyperplasia and lobular carcinoma in situ are linked to an increased risk of breast cancer.
- Parent or sibling with breast cancer
You’re more likely to acquire breast cancer if you have parents, siblings, children, or other close relatives who had been diagnosed before.
- Inherited gene mutations
Approximately 5% to 10% of breast cancers happened by single faulty genes passed down from parents to children, which we can detect through genetic testing.
BRCA1 and BRCA2 mutations: The most common cause of the hereditary disease is an inherited mutation in the BRCA1 or BRCA2 gene. In normal cells, these genes help to produce proteins that repair damaged DNA. Mutations in these genes can result in abnormal cell proliferation, which can lead to cancer.
- Alcohol use
Alcohol consumption is linked to an increased risk of some forms of breast cancer, according to research.
- Overweight or obesity
Obesity increases the likelihood of developing breast cancer and having it return.
Screening for breast cancer

Breast self-exam
A breast self-exam is a self-examination of your breasts to raise awareness of breast cancer. To help raise breast awareness, you use your eyes and hands to detect changes in the appearance and feel of your breasts. If you notice any new changes in your breasts, consult your doctor. Even though the majority of breast changes found during a breast awareness self-exam are natural, some changes can indicate something a little more serious, such as breast cancer.
Routine breast self-examinations are not preferred as part of the screening by most medical organizations. Because breast self-exams haven’t been demonstrated to be beneficial in identifying cancer or extending the lives of women with breast cancer, they’re not recommended. However, experts feel that women should feel familiar with their own breasts so that they can recognize what is normal and report corrective action, they can take.
Also Read:- Breast Infection (Mastitis) : Home Remedies
Clinical breast exam by your healthcare provider
A clinical breast exam (CBE) is a physical examination performed by a medical professional. It’s usually done as part of a routine medical examination. A healthcare provider should perform a CBE who has had extensive training in the procedure. This could be a doctor, nurse practitioner, or another member of the medical team. This training is not available to all health care providers.
A professional health care practitioner should feel your breasts, underarms, and the area just below your collarbone (breast bone) for any changes or abnormalities, such as a lump, according to the National Comprehensive Cancer Network (NCCN). Your breasts should be visually checked while you are sitting up and physically examined while you are lying down by your health care practitioner. If a CBE is not performed at your check-up and you want one, ask your doctor to perform one for you (or refer you to someone who can).
Screening mammogram
The average screening mammography patient has no symptoms and a moderate risk of breast cancer. For example, there is no family history of the disease and no visible lumps. The screening mammography serves two functions in this case: To look for any problems in the tissue, and to Establish a basis for future treatments to monitor breast tissue changes.
This patient is also undergoing the standard breast cancer screening procedure: When someone becomes 40 and has no family history of breast cancer, they should continue the checkup once a year. Patients with a family history of breast cancer, especially first-degree relatives, should continue screening 10 years before their relative had diagnosed. Individuals over the age of 30 who are at risk genetically should go for check-ups at least once a year. The average screening mammography takes 10 to 15 minutes, and there is usually no supervising doctor present. For insurance purposes, the Affordable Care Act stipulates that screening mammograms for women aged 40 and up shall be free of charge, with no out-of-pocket payments.
We can request additional views for screening mammography in addition to the normal process, especially if a patient has breast implants, is in pain, or has other positioning issues.
Diagnosing mammogram
Diagnostic mammography will be requested if abnormalities are discovered during the screening. If a patient has seen or screening mammography has found the following indications, this procedure will determine if they point to breast cancer:
- Lumps
- Tumors that aren’t large enough to sense
- In situ duct carcinoma (DCIS)
- Breast soreness, nipple discharge, or thickened skin are all possible causes.
Why has the size or contour of a breast changed?
This technique will work as a follow-up to regularly assess breast tissue for individuals who have already had a diagnostic exam or have had breast cancer.
Diagnostic mammography, as an imaging procedure, provide more detail through extra pictures or views, such as spot compression or spot compression with magnification, and can provide you with more information about abnormalities found during a screening. As a result, these factors can help with a more accurate diagnosis or the recommendation of additional diagnostic tests such as a biopsy or ultrasound.
Diagnostic mammography takes longer than screening mammograms because of these considerations, but they normally last no more than 30 minutes. While the patient is still in the clinic, a diagnostic radiologist evaluates the images and may request more photos with magnification if the process reveals any abnormalities or other areas of concern.
Breast ultrasound
Breast ultrasound is a type of imaging exam that looks at the inside of your breasts using sound waves. It can assist your doctor in detecting breast issues. It also allows your doctor to observe how well blood is circulating to different parts of your breasts. When a doctor see a change on mammography or when a change is felt but not visible on a mammogram, this test is frequently utilized.
Breast MRI
Magnetic resonance imaging, or MRI, is a technique that produces comprehensive cross-sectional images of the inside of the body using magnets and radio waves. Because MRI does not employ X-rays, there is no risk of radiation exposure. Breast MRI has a variety of applications in the treatment of breast cancer, including:
- Screening of Women at high risk is important. (women who have known to have a higher-than-average risk is due to strong family history or a genetic anomaly)
- obtaining additional information on a suspicious spot discovered on a mammogram or ultrasound
- After therapy, keep an eye out for recurrence.
Having a breast biopsy
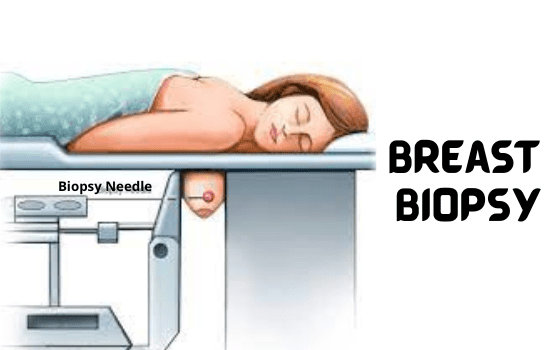
A breast biopsy is a clear and simple medical procedure that involves the removal of a sample of breast tissue and sending it to a lab for testing. A breast biopsy is the most accurate approach to determine whether a suspicious lump or area of your breast is malignant.
Breast lumps aren’t necessarily malignant, so keep that in mind. A variety of disorders can cause breast lumps or growths. A breast biopsy can identify whether a lump in your breast is malignant or benign (noncancerous).
Analyzing the breast biopsy
A health care professional will examine the breast biopsy tissue under a microscope and perform specific tests. Their report will let you know if you have cancer and if it grew because of estrogen receptors, progesterone receptors, or human epidermal growth factor receptor 2 on a cancer cell. The results of these tests will help your doctor to choose the right tests.
Understanding the behavior of Breast Cancer
- Non-invasive
Cancer cells that are not invasive are discovered in the lobules or ducts. They haven’t migrated beyond the breast tissue or to the lymph nodes.
- Invasive
Invasive breast cancers are tumors that have spread to the surrounding breast tissue.
- Recurrent
Its recurrence occurs when cancer returns after therapy and has gone undetected for a period of time. After the treatment of original breast cancer, recurrence might occur months or years later.
- Metastatic
Breast cancer that has spread to other parts of the body is referred to as Stage 4 cancer. It can affect other regions of the body by malignancy. Commonly affected organs include the lungs, liver, bones, and brain.
Common Types of Breast Cancer
- Invasive ductal carcinoma
IDC is the most common type of breast cancer. Invasive ductal carcinomas account for approximately 8 out of 10 (or 80%) of all breast cancers. IDC starts in the ducts and spreads to the surrounding breast tissues. IDC can spread to the lymph nodes and possibly other parts of the body if not addressed.
- Invasive lobular cancer
The most common kind of breast cancer is ILC. ILCs account for about one in every ten cases of breast cancer. ILC begins in the breast lobules (milk-producing glands) and spreads to surrounding breast tissue. ILC can spread to the lymph nodes and possibly other parts of the body if not addressed.
Less common types of Breast Cancer
- Inflammatory breast cancer
IBC is a unique and deadly type of invasive breast cancer. Because cancer cells block lymphatic vessels in the skin, IBC has some inflammatory symptoms such as redness and swelling. Other symptoms of IBC include dimpling or redness of the skin in the breast (similar to orange skin), a lump in the breast or armpit, pain in the breast or nipple, release from the nipple, or a nipple that turns inward (inverted nipple).
- Tubular breast cancer
Breast cancer in the form of tubular carcinoma. It’s a form of ductal carcinoma that’s invasive (IDC). Tubular carcinomas acquire their name from the tube-shaped features that they can see under a microscope in the tumor. The tumors are usually 1 cm in diameter or smaller, and they grow slowly. Tubular carcinomas are a type that is uncommon. They make up about 1% to 5% of all IDCs in the breast. In men, tubular carcinoma is uncommon. Women are on average 50 years old when they are diagnosed with cancer.
- Colloid breast cancer
Colloid breast cancer is an uncommon kind of invasive ductal cancer stated as an excessive mucous deposition. It is a slow-growing malignancy that primarily affects older women. Estrogen and progesterone receptors are expressed in colloid breast cancer, although Her-2 is absent. The best surgery and adjuvant treatment for this are unknown.
- Metaplastic breast cancer
Metaplastic breast cancer (MBC) is an uncommon type that accounts for less than 1% of all cases each year. MBC is distinguished by the wide range of cell types that make up the tumor, which can make diagnosis challenging. Furthermore, MBC has the potential to be more aggressive than other kinds of breast cancer.
What is triple-negative breast cancer?
Triple-negative breast cancer means the tumor has no estrogen, progesterone, or HER2 new protein receptors on the surface. The triple-negative disease may have the worst outcome and often requires more intensive treatment.
Stages of Breast cancer

- Breast cancer in its early stages
DCIS is the first stage. DCIS cancer cells have been confined to the breast ducts and have not spread to nearby tissue.
- Stage 1
Cancer cells have spread to neighboring breast tissue.
- Stage 2
The cancer cells are either less than 2 centimeters in diameter and have spread to the underarm lymph nodes, or it is more than 5 centimeters in diameter but has not spread to the underarm lymph nodes. Tumors at this stage can range in size from 2 to 5 centimeters in diameter and may or may not affect nearby lymph nodes.
- Stage 3
At this point, cancer has spread beyond its original site. It has infiltrated nearby tissue and lymph nodes, it has not spread to distant organs. Stage III calls it locally as advanced breast cancer.
- Stage 4
Cancer has spread to other parts of your body, including your bones, liver, lungs, and brain. Stage IV calls it metastatic breast cancer.
Grades of breast cancer
- Grade 1
The cancer cells resemble normal tissue the most and grow slowly (well-differentiated).
- Grade 2
The cancer cells have graded between 1 and 3 on a scale of 1 to 3. (moderately differentiated).
- Grade 3
The cancer cells have an unusual appearance and are rapidly developing (poorly differentiated).
When the tumor grade is higher, the prognosis is worse for any given tumor size and stage of breast cancer.
Treatment of Breast Cancer

Breast cancer treatment depends on the type and the stage of your cancer. You will need treatment from the cancer specialized people from a different area of the stream.
The main treatment includes
Surgery
Common types of surgeries to remove the tumor are
- Lumpectomy
- Simple mastectomy
- Modified radical mastectomy
- Prophylactic mastectomy
- Mastectomy with reconstruction
- Sentinel lymph node biopsy
- Axillary node dissection
- Radiation therapy
Radiation therapy is the use of radiation energy to kill cancer cells. It is mostly recommended after surgery or chemotherapy
Chemotherapy
Chemotherapy uses drugs to destroy cancer cells. It can refer as an IV or pill. Chemotherapy can be used to shrink a tumor before surgery called neoadjuvant chemotherapy, kill cancer cells after surgery called adjuvant therapy, and control Medi statistics breast cancer called palliative chemotherapy.
Hormone therapy
Hormone therapy will recommend only if your tumor is positive for the hormones estrogen and progesterone. It can lower the risk of coming back and help shrink or slow the growth of Medi statistics estrogen receptors breast cancer. Tamoxifen and aromatase inhibitors are common hormone therapies for breast cancers.
Targeted therapy
Targeted therapy uses drugs or other substances to identify and fights specific types of cancer cells with less harm to normal cells. These therapies stop cancer cells from growing, identify and kill cancer cells and increase the immune system’s attack on cancer cells.
Survivorship
After the treatment, patients with breast cancer face new obstacles. They set out to discover what is generally referred to as their new normal. Survivors’ lives will never be the same again, physically, mentally, or socially. The first year after therapy is the most crucial year for the cancer patient. Post-chemotherapy side effects commonly cause fatigue, neuropathy, and cognitive impairment in survivors. Some patients experience despair and anxiety, as well as a constant worry of relapse. The survivors frequently report feelings of isolation from society and difficulty readjusting to traditional social norms.
The current breast cancer surveillance model focuses on the physical aspects of care and early detection of recurrence while ignoring the mental and emotional aspects of care4. According to reports, survivors have to go through unnecessary and excessive testing at times, with a wide range in the quality of care provided by the physicians who followed up on these patients.
Getting diagnosed with breast cancer can be frightening, frustrating, and even depressing. If you or a loved one is suffering from this disease, it is critical that you take advantage of the numerous resources available to you. Discuss your medication options with your healthcare professional. Before making a decision, you may want to seek a second opinion. You should feel encouraged by your treatment plan. Finally, joining a local support group can alleviate feelings of isolation and allow you to communicate with others who are going through similar experiences.
Today, people are living 5, 10, or even more years due to advancements in cancer treatment. Many trials are happening to treat these cancers, and there is also a trial that made history
Also read: Surprising Benefits of Massage Therapy




