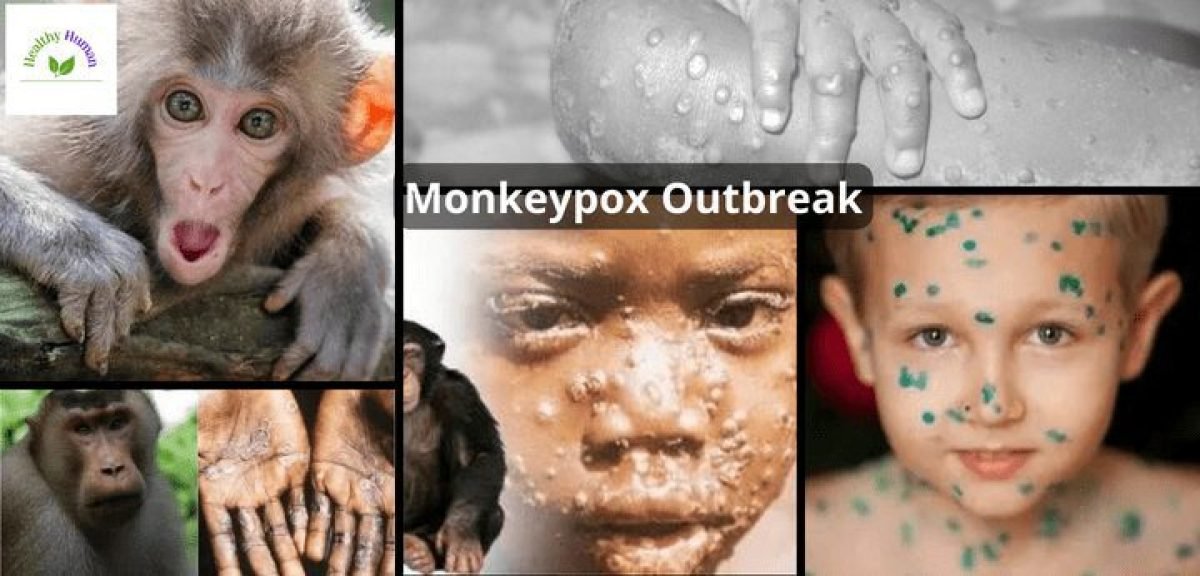
We have seen first-hand how rapidly a pathogen may devastate civilization thanks to the coronavirus epidemic. Due to COVID 19, so much has changed in only the past two years. And a lot of people worry that we could soon see another pandemic on the scale of COVID. There has been a lot of discussions recently regarding monkeypox and a potential epidemic.
About Monkeypox
The monkeypox virus may infect people, leading to the illness known as monkeypox. It is a member of the orthopoxvirus family, which also includes smallpox, vaccinia, and cowpox viruses. The early 1950s saw the discovery of monkeypox. due to two outbreaks of a disease similar to the pox among laboratory monkey groups. Thus, the term “monkeypox.” In the 1970s, monkeypox was first discovered in a human being in Africa. Since that time, the illness has remained endemic, or primarily restricted to particular parts of Africa.
Monkeypox Variants
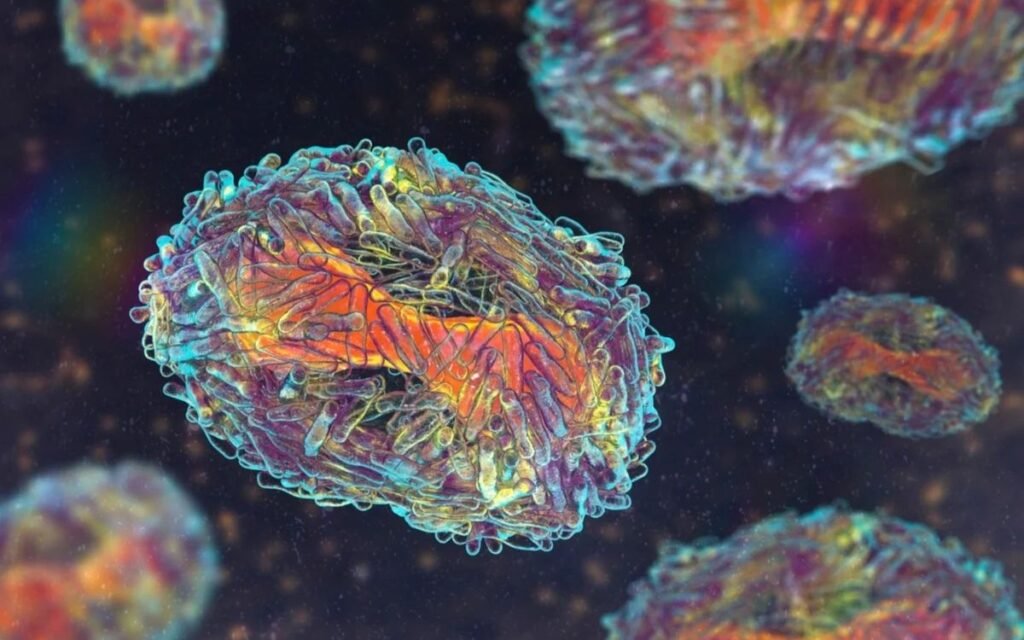
The Congo basin clade and the central Africa clade are the two primary subvariants of the monkeypox virus. The Congo basin type is call it as more contagious and has traditionally caused more serious illness. However, monkeypox is far less contagious than its relative smallpox, and the symptoms are often much less severe.
Initial 1-3 days of symptoms
The first one to three days is similar to other viral diseases, marked by fever, chills, exhaustion, headache, muscular pains, and enlarged lymph nodes. Infected people then begin to develop a rash that grows from tiny, flat lesions to finally huge, fluid-filled blisters. These blisters will drain, scab up, and finally fall off during the following few weeks.
The illness often lasts between two and four weeks before going away on its own and is self-limiting, meaning that it normally goes away on its own. However, other people have far more severe symptoms and grow more serious conditions. Such as pneumonia, sepsis, and secondary infections, to mention a few.
The CDC estimates that up to 1 in 10 Africans who have monkeypox pass die as a result of the illness.
But the issue still stands: why are we so worried about monkeypox today.
The cause is that the virus starts to spread outside of Africa, controlled for decades, in the form of several new cases.
Historical Transmission Methods
In the past, the animal-to-human transmission of monkeypox was the main method. such as from a rat or a dormouse. The person could later infect one or more members of their immediate family. However, traditionally, the illness has dissipated swiftly. Transmission between humans believe to happen mostly through direct touch, by big respiratory droplets, or through contact with bodily fluids or lesions.
Due to historically low transmission rates, it has sometimes been possible to stop the fact that the disease is not spreading. According to its typical course is what is driving the present epidemic to be so disruptive. And more people are developing monkeypox infections, most likely as a result of human interaction.
But are you supposed to be worried about yourself or your loved ones and is all the uproar surrounding monkeypox justified?
Healthcare Access
According to the WHO, the majority of patient symptoms have been rather moderate, and the case fatality rate for monkeypox, thought to be between three and six percent. With these data, there is, however, a crucial component to take into account.
In parts of Africa where monkeypox is a more widespread disease. Access to healthcare is frequently restricted. Supportive therapy, such as antipyretics, antibiotics, oxygen fluids, and close observation. It can be used to treat severe viral disease consequences such as sepsis and secondary infections.
In essence, patients merely require a little bit of additional assistance as their bodies heal from the sickness. Additionally, there are some drugs use to treat more severe instances of monkeypox, such as the antiviral drugs tecovirimat and Brin cidofovir. Due to these factors, nations with better access to healthcare may not have a case fatality ratio of three to six percent.
However, having monkeypox and without access to supportive treatment is one reason why the recent increase in COVID cases has been so alarming. Access to care may suffer if hospital systems are overburdened with patients. And are lacking a buffer. causing individuals to pass away who might not have otherwise.
This is true even if the predicted three to six percent case fatality rate for monkey boxes is not reachable. Depending on the nation, the case fatality ratio of COVID-19 has expectation to range from 0.5 to 3. And the number of fatalities is visible.
The Transmission Method of Monkeypox
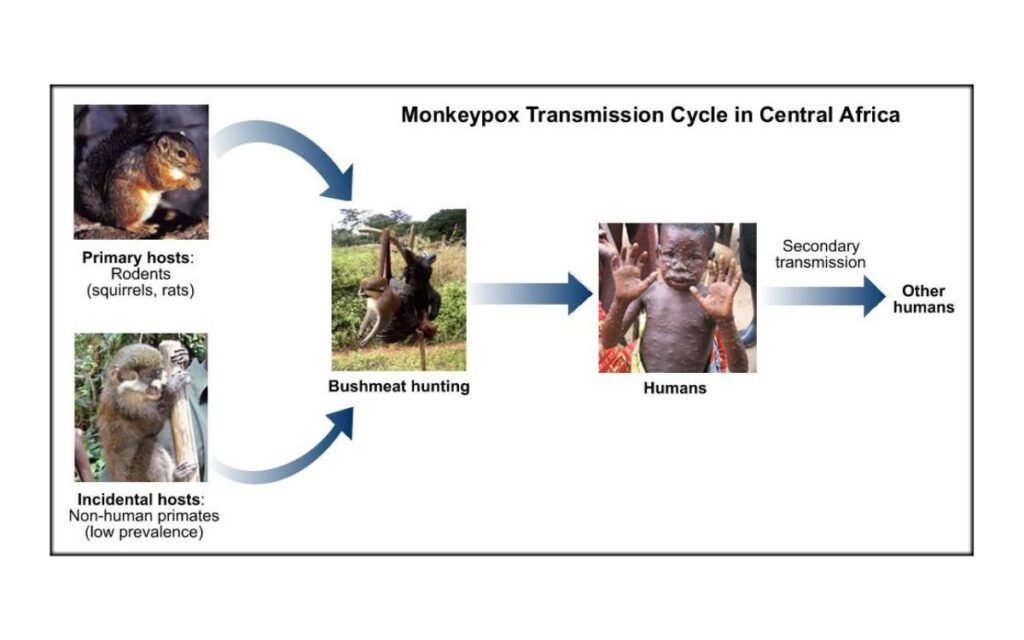
The problem with covid 19 is that it spreads amongst people quite quickly. Tiny respiratory droplets from an infected person’s cough, sneeze, or even merely talking can spread the virus. Anybody nearby can subsequently inhale those little droplets into their lungs and get an infection. Coronavirus can consequently spread widely across a population.
However, monkeypox does not spread in this manner. Large respiratory droplets, bodily fluids, and lesion material, assumed to be the main means of transmission from animal to human or human to human. For instance, a 2007 research discovered that handling an infected animal, scratched by an infected animal. Or changing an infected animal’s bedding were all linked to a higher chance of having monkeypox.
On the other hand, there was no connection between the development of monkeypox and indirect exposures. Such as being close to an infected animal, which is defined as being within six feet of that animal without touching it. As a result, monkeypox is not as contagious as, say, covid, which is easily transferrable by being in close contact with an infected person. In the past, monkeypox required direct physical touch.
Also Read :- Impact and Control of Zoonotic Diseases on human Health
Values of Ro
By comparing the Ro values of covid and monkeypox, we can understand how big of a difference this form of transmission makes. The Ro value describes the typical number of persons to whom each sick person is anticipated to spread the illness. This figure essentially examines the spreadability of an infectious illness. A Ro of two to three was predicted for the original Covid 19 version. An estimated Ro value for the more contagious delta version is between five and seven. And the Ro for the more modern Omicron form has a thought to reach eight.
This means that each person who contracts the omicron version of the coronavirus, thought to infect about eight more persons. Then each of those eight individuals may anticipated to spread the infection to an additional eight individuals, and so on. The coronavirus was able to spread so swiftly because of this. Most estimates of recent outbreaks of monkeypox are not comparable to or less than one.
The virus isn’t propagated well enough via people for it to be able to sustain itself in the community, which means that some monkeypox patients don’t even infect a single person. The virus has remained mostly indigenous to Africa because of this.
And the majority of cases have been caused by animal to human transmission. Close relatives or medical professionals who are caring for patients who have monkeypox are frequently at risk for contracting the disease from another person. And even then, it appears that using the right contact precautions can significantly reduce a lot of that danger. But why are there so many instances now if it’s not that simple to spread from person to person?
Causes of Monkeypox Cases
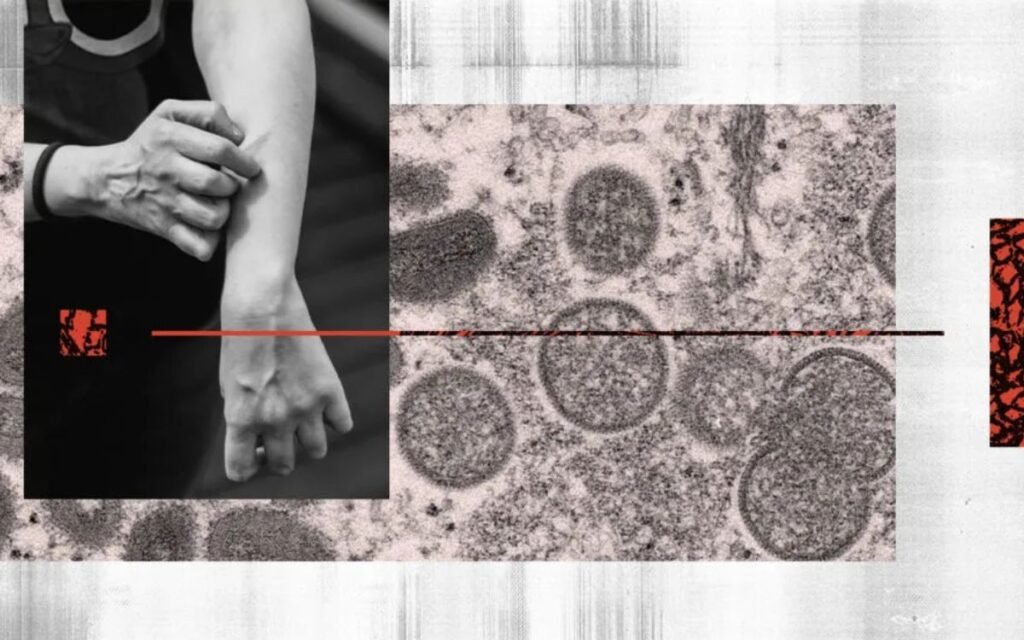
Perhaps a mutation The main cause for concern is that the virus has altered, making it easier for people to contract it, which is why there are more instances now. According to reports, research is presently being done to determine whether the monkeypox genome has changed. There are no unique mutations, according to a preliminary study from Mount Sinai’s Icon School of Medicine. However, additional study is still required.
DNA and RNA Viruses
But compared to a virus-like covid 19, monkeypox is far less likely to change given its nature. DNA viruses include orthopox viruses like monkeypox. This contrasts with RNA-based pathogens like the flu or coronavirus. DNA and RNA are essentially biological instruction manuals, in case you forgot from general biology. Generally speaking, DNA serves as a template for the creation of RNA, which in turn serves as a template for the creation of various proteins, each of which performs a particular function.
The machinery that our cells employ to make and copy DNA and RNA has taken over by viruses. When they enter our body and infect healthy cells And they utilise it to produce more identical duplicates of themselves instead. The virus duplicates its genome to make a copy of itself repeatedly, hence these replication processes are not flawless. There is a chance for errors to occur; these are call it as mutations.
Even though they are random, the virus’s interactions with other cells may occasionally has a impact by these errors in the genome. The issue now is that these alterations can make it simpler for a virus to spread from one person to another. As RNA replication machinery is not particularly adept at spotting or correcting errors. RNA viruses like the flu and covid have significant rates of mutation.
However, the machinery involved in DNA replication is far better at spotting and correcting errors. In fact, it is around 100 times more effective than RNA at identifying and correcting errors. This indicates that compared to RNA-based viruses, DNA-based ones are often significantly less prone to experience mutations. Additionally, mutations are sporadic even when they do happen.
Therefore, it is also unlikely that a mutation would have arisen that would benefit the virus in some way.
Transmission of monkeypox among gay and bisexual

The recent spread of this outbreak outside of Europe is probably due to a few significant raves that took place there. That drew in a large worldwide following. Young males who are either homosexual or bisexual or who have sex with men have made up a sizable number of those infected with monkeypox and have no prior history of traveling to Africa. Authorities in Portugal and Spain also said that their instances usually involved males who had intercourse with other guys. And that the infections were discovered when the men went to sexual health centers for the treatment of their sores.
Although it is not understandable how monkeypox spread during sex, intimate physical contact during sexual activity call to adequate for monkeypox transmission. Even in the worst-case scenario, there may be a change in the monkeypox genome that makes it easier for people to contract the disease from one another.
How would that affect us? Could it possibly start a new pandemic?
Although not impossible, it is also not very plausible. In fact, monkeypox outbreaks have occurred in our country before. A monkey box epidemic occurred in the Midwest of the United States in April 2003. A consignment of rodents, including several kinds of mice, rats, and squirrels, afflicted with monkeypox, came from Ghana. These mice were kept with prairie dogs at an animal dealer when they arrived in the country. And later sold as pets The monkeypox virus moved from the prairie dogs to their owners once it came into contact with people.
At that time, every person who had monkeypox had contracted the illness through contact with sick prairie dogs. There were no cases that were solely attributable to interpersonal interaction.
CDC and other Agencies’ efforts
In collaboration with other governmental organizations, the CDC and public health departments conducted comprehensive lab testing. Created recommendations for medical professionals, veterinarians, and others who handle animals and looked into human instances. They also distributed smallpox vaccinations and remedies.
Testing for monkeypox
- Monkeypox symptoms may resemble those of other infections (e.g. chickenpox). A health professional’s evaluation and a viral test are necessary to determine whether someone has monkeypox.
- If you have undergone a monkeypox test, wait for the findings before engaging in personal contact, including sex, at gatherings, places, and activities. If your test is positive, continue as follows: The advice of your healthcare practitioner and the local public health authority
Smallpox Vaccine for Monkeypox
Keep in mind that smallpox and monkeypox are members of the same viral family. It has established that the smallpox vaccination is effective against monkeypox. The CDC estimates that the smallpox vaccination is at least 85% effective in preventing monkeypox based on historical evidence from Africa. In the United States, everyone received the smallpox vaccination as a new-born until the 1970s.
Smallpox, eradicated in the end, therefore we ceased administering the vaccine because it was no longer necessary. The majority of Americans over 50, born here most certainly received the smallpox vaccination as a kid. And as a result have some level of immunity against monkeypox. Anyone under the age of 50, however, probably not immunized against smallpox. Despite this, doctors still have plenty of the vaccine on hand in case a situation calls for its usage.
Other Vaccinations
In fact, since then, scientists have even created a vaccination that is even more effective. The smallpox vaccine previously made with the vaccinia virus, a member of the orthopoxvirus family. It was a live attenuated virus, therefore there was a tiny danger despite its tremendous effectiveness. That anyone who got the vaccination would die as a result of the vaccinia virus’s unchecked replication.
In the United States, problems between 1959 and 1968 resulted in 68 fatalities. Even said, it’s still a very small portion of the population when you take into account that everyone was receiving the vaccination. Since then, scientists have created a vaccination that carries a far lower risk of side effects.
It’s doubtful that medical professionals will have to resort to mass immunisation campaigns with the smallpox vaccine, as they did with COVID 19. Even if monkeypox instances continue to climb.
Instead, given the virus’s low transmissibility, merely concentrating on people at high risk of transmission will probably be sufficient to prevent the virus’s spread.
Self Care Suggestions
Here are some straightforward self-care suggestions if you test positive for monkeypox.
• If you have the monkeypox, avoiding close contact with other people, including sex, can reduce your risk of transmitting the disease. If at all possible, lock yourself in a room and heed the advice of your doctor and the relevant regional health authorities.
• Talk with your doctor about how to inform those you were in close touch with before being diagnosed; and
• When it comes to therapy, adhere to the advice of your doctor (no special treatment is typically necessary). Maintain the cleanliness of the rash-affected regions to take good care of your skin. If the rash itches, get medical treatment and wash with a block of mild soap. Keep in mind to wash your hands completely after handling the rash.
This will help to prevent infections and their effects. If you see swelling or redness around the rash, or if you develop a fever despite your symptoms appearing to be improving, get medical help right once.
• If you think you might need it, get help with your mental health.
When to see a doctor
These characteristics make it highly improbable that this will develop into a new pandemic; instead, it is more likely that it will just fade out in the upcoming months. Despite this, it’s still vital to be aware of monkeypox, especially if you belong to a group that is more susceptible to infection or complications. Or if you reside in a region where there are many instances.
Additionally, you should see your doctor and get a look out for if you have a vesicular rash, fever, body pains, lethargy, enlarged lymph nodes, or any of these symptoms. Even Nevertheless, it might be frightful to read news stories about the next virus or sickness, such as monkeypox. Always make an effort to distinguish between the signal and the noise.